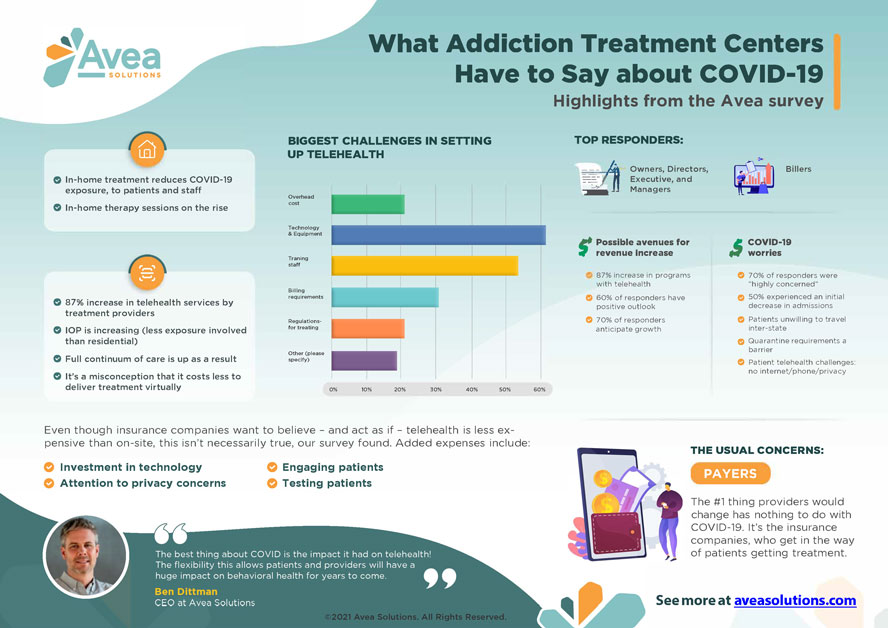
We are excited to announce KIPU has joined forces with Avea Solutions so treatment centers no longer need to compromise when choosing their core systems. This is a huge opportunity for Avea to invest substantially in additional resources that will support treatment centers in growing their businesses, speed up our ability to roll out new product improvements and extend new offerings that solve some of our customer’s biggest challenges.
Necessity is the mother of invention – or perhaps in these times, a reinvention of your practice. There are rapid changes being made at the federal and state levels to expand options for telehealth in the Behavioral Health and SUD space so that patients can continue to receive essential healthcare during this crisis. With technology, it’s possible to continue your life-saving programs and we’re here to help you through the transition.